Prior Authorization Support (PAS): Modern, Standards-Based Prior Authorization is Coming!
The need for efficient, scalable prior authorization has never been greater.
- The average physician handles 39 prior authorizations per week
- Physicians and their staff spend ~13 hours per week on related administrative work
- 97% of providers report delays or denials for necessary care due to PA requirements
- 20% of physicians say they always appeal adverse decisions
These numbers highlight a system under strain, where administrative burden slows care delivery, increases costs, and creates friction across the payer-provider relationship. PAS is designed to address this challenge.
Beginning January 1, 2027, payers are mandated by CMS to implement electronic, standards-based prior authorization processes to improve decision turnaround times, limit delays in care, and reduce administrative burden and costs. Specifically, CMS-0057-F extends payer interoperability requirements to require Prior Authorization Burden Reduction for their government subsidized lines of business, and some states requiring the same for pharmacy prior authorization as well. As part of this mandate, payers must expand the Patient Access API to include prior authorization information, enable data sharing with in-network providers through the Provider Access API, and support member data exchange between payers via the Payer-to-Payer API. In addition, they are required to implement Prior Authorization APIs that support electronic submission of requests, along with the exchange of criteria, status, and decision responses.
Powering Prior Authorization from Intake to Decision Notification
PAS refers to the FHIR-based Prior Authorization Support APIs that are mandated by CMS-0057-F. PAS powers the exchange of information between payers and providers, driving decisions forward, and ensuring that prior authorization requests move efficiently from submission to decision notification.
PAS is a set of FHIR-based, standardized APIs that enable providers to submit prior authorization requests and supporting documentation electronically to health plans. PAS enables structured, complete data exchange between providers and payers, supporting automated workflows that reduce manual intervention and administrative burden. By ensuring consistency and completeness in submissions, it drives faster, more reliable decision-making while also enabling organizations to scale compliance with CMS interoperability and prior authorization mandates. Importantly, PAS also supports near real-time visibility into authorization status, including timely access to decision outcomes and detailed denial reasons, enabling providers to take faster, more informed action.
Just as importantly, PAS helps eliminate the inefficiencies of traditional processes like fax, portals, and fragmented communications, that create delays and rework. However, like many interoperability standards, PAS on its own is not enough.
Opala PAS: Beyond API Connectivity to End-to-End Prior Authorization Orchestration
To truly deliver value, organizations must be able to:
- Orchestrate workflows across systems
- Ensure data completeness and accuracy
- Integrate seamlessly into clinical and operational processes
- Manage exceptions, updates, and downstream actions
This is where many organizations struggle, and where the right platform makes all the difference. Opala has transformed PAS from a technical standard into a fully operational, scalable solution. Built on the HealthSynq™ platform, Opala’s PAS capabilities go beyond basic API connectivity to deliver end-to-end orchestration of the prior authorization process.
With Opala, organizations can:
- Streamline submission and data exchange: Submit complete, FHIR-based requests aligned to payer requirements to reduce rework and delays.
- Orchestrate workflows across systems: Integrate PAS into broader workflows, connecting intake (CRD), rules evaluation, submission, and response handling into a unified experience.
- Reduce administrative burden: Automate submission and follow-up to cut manual work for providers and staff.
- Accelerate time to decision: Improve submission quality and automation to speed determinations and scheduling.
- Support compliance at scale: Stay aligned with CMS requirements while adapting quickly as rules evolve.
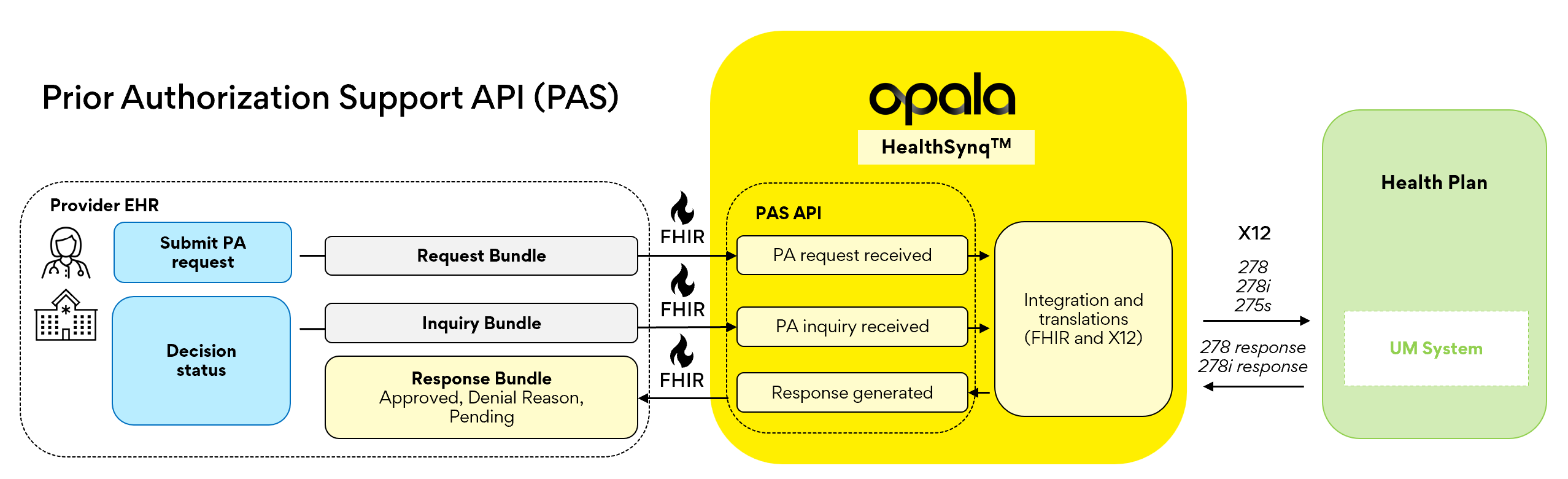
Bringing It All Together
Modern prior authorization requires more than point solutions, it requires a connected, end-to-end approach.
- Digitized Prior Authorization Rulesets provide the structure
- CRD enables intelligent intake by providing the requirements prior to a submission
- PAS ensures an accurate and timely determination and notification process so that necessary care can be scheduled without delay
PAS ensures that prior authorization that patients get the care that they need without delay and that providers can focus on the patient instead of paperwork. With Opala, payer organizations can move beyond fragmented, manual processes and toward a future where prior authorization is fast, smart, compliant, and truly aligned with the needs of patients, providers, and payers.
Prior Authorization and Pre-Claim Review Program Stats for Fiscal Year 2024. September 16, 2025 CMS

