Connecting Blue Plans to the Future of Interoperability

How Opala Enables Seamless Exchange Through the BCBSA Interoperability Hub
Healthcare interoperability is rapidly evolving, and with it, the expectations placed on health plans. Providers increasingly expect real-time access to coverage and clinical data, while regulators are pushing the industry toward standardized, API-driven exchange. At the same time, Blue Cross Blue Shield plans must ensure that critical data can move seamlessly across plan boundaries when members receive care outside their home service area.
The BCBSA Interoperability Hub represents an important step forward in solving this challenge.
Designed to support secure, standardized data exchange across the Blue ecosystem, the hub enables plans to share clinical and coverage information while supporting modern prior authorization workflows. At Opala, we’re excited to help our customers connect to the Interoperability Hub and participate fully in this next phase of healthcare interoperability.
Why the BCBSA Interoperability Hub Matters
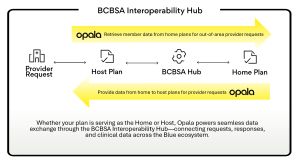
Healthcare data exchange is challenging even within a single organization. When members receive care outside their home plan’s geographic service area, as frequently occurs through the BlueCard® program, the complexity increases even further.
Providers still need timely access to clinical and coverage information to guide treatment decisions, while health plans must ensure accurate and compliant data exchange between “home” and “host” plans. Historically, these interactions have relied on fragmented processes that can introduce delays, administrative burden, and unnecessary friction for both providers and plans.
At the same time, regulatory changes are accelerating the industry’s shift toward standardized, API-driven interoperability. New requirements are pushing health plans to modernize how they exchange clinical data and manage prior authorization workflows using FHIR-based standards.
The BCBSA Interoperability Hub was created to address these challenges by providing a shared delivery platform that enables secure, standardized data exchange across the Blue ecosystem.
The hub provides the software infrastructure, standardized data formats, procedures, and governance framework that allow Blue Cross Blue Shield plans to exchange industry-standard transactions supporting prior authorization, clinical data exchange, Provider Access API capabilities, and BlueCard out-of-area member support. Leveraging HL7 Da Vinci FHIR® Implementation Guides, the hub enables plans to exchange information using modern interoperability standards while maintaining consistency and compliance across the network.
By centralizing these exchanges through a common platform, the Interoperability Hub reduces the complexity of plan-to-plan data sharing while helping ensure that providers can access the information they need to support timely, coordinated care.
Easy Implementation with Opala
Opala enables health plans to connect to and participate in the Interoperability Hub through the HealthSynq™ interoperability platform. By managing hub connectivity and transaction workflows on behalf of our customers, Opala simplifies the operational complexity of participating in the Blue network’s interoperability framework.
Provider Access API Support
Opala enables customers to retrieve and exchange clinical data for BlueCard members by:
- Routing provider requests for out-of-area members through the Interoperability Hub
- Retrieving data from the member’s home plan
- Returning that data to the requesting provider via the Provider Access API
Opala also supports inbound requests from other Blue plans, enabling customers to provide clinical data for their home plan members through the hub. Data received for home plan members can be stored within the HealthSynq™ data platform, creating a more complete and accessible data environment.
Prior Authorization Workflow Support
Opala also supports digital prior authorization transactions through the hub, including:
- CRD requests to identify coverage requirements
- PAS transactions for authorization submission and response
By enabling these capabilities through HealthSynq™, Opala ensures that prior authorization workflows remain compliant, consistent, and interoperable across the Blue ecosystem.
Learn More
If your plan is preparing to connect to the BCBSA Interoperability Hub or evaluating how to support Provider Access and digital prior authorization workflows, Opala can help.
Contact our team to learn how the HealthSynq™ platform enables seamless hub connectivity while simplifying compliance with Blue Association and federal interoperability requirements.